

Spinal infections are usually the result of bacterial or fungal infections from other places in the body that spread to the spine though the bloodstream (hematogenously). Less commonly, they occur from local extension of a neighboring infection (eg, psoas abscess). Spinal infections are usually categorized by their location as discitis (infection of the vertebral disc space), vertebral osteomyelitis (infection of the vertebral body), and epidural abscess (infection of the spinal canal space). Vertebral osteomyelitis is the most common, with an estimated prevalence of 2.4 cases per 100,000 persons. The risk increases with age, and accounts for 4% to 6% of all cases of osteomyelitis. Epidural infections are relatively rare (0.2 to 1.2/10,000 hospital admissions), but are more likely to require emergent surgical treatment and are associated with significant morbidity and mortality rates.1,2,3
Postoperative wound infections and adverse events are relatively rare but are predictable risks and consequences of surgery. Although the absolute number is small in comparison to the volume of cases overall, they tend to have a disproportionate impact on both patient outcome and societal cost. There are many potential adverse events reported with any procedure, and the frequency and severity of these events varies based upon both patient and disease-specific variables. The codes included for query of the various databases for wound infections and adverse events are 996.2 (mechanical complication of nervous system device/implant), 996.59 (mechanical complication due to other implant/device), 996.63 (infection due to nervous system device/implant), 996.75 (other complications due to nervous system device/implant). Postoperative infections were queried for codes 998.51, 995.59, and 998.60. No differentiation was found in rates of infection between the spine and other areas within the body.
The most common adverse events associated with spine surgery include neurologic injury, infection, re-operation, medical complications, and dural tear.1 Of these, infection is the most frequently studied and reported both in the literature and within healthcare delivery organizations. Infection rates for lumbar spine surgery are frequently reported between 3% to 5% in many studies, but have a wide range depending on the type of procedure performed. Studies have reported an infection rate of 1% or less in single-level micro-discectomy cases (a small decompression procedure for disc herniation with sciatic pain); 3% to 7% in instrumented fusion cases (a stabilization procedure usually involving one to two levels for back pain or instability); 7% to 10% in adult deformity reconstruction (procedures to realign the spine in patients with scoliosis/kyphosis); and greater than 20% in neuromuscular deformity cases.1,2,3,4
In 2011, a total 370,000 discectomy and 498,700 fusion/refusion procedures were performed. Based on conservative estimated infection rates of 1% and 5%, for discectomy and fusion/refusion, respectively, we can estimate there were 28,600 postoperative spine infections. It is unknown what proportion of spinal infection diagnosis-related health care visits this represents. (Reference Table 2.14 PDF [1] CSV [2] and Table 2.19 PDF [3] CSV [4])
Risk factors associated with postsurgical complications and infection following spine surgery include obesity, diabetes, steroid and alcohol use, revision surgery, age, and operative time and blood loss. Postsurgical wound infections can arise from direct inoculation of the wound intra-operatively or indirectly by hematogenous seeding from other sources (ie, spread through the bloodstream). The most frequent organism cultured is Staphylococcus aureus (Staph infection), while gram-negative organisms are more commonly seen in polymicrobial infections (infections involving multiple types of bacteria).1
The most frequently reported symptoms are back pain, fever, and wound drainage, usually within the first 10-20 days of surgery, although latent infections may occur more than one year from surgery.
Superficial infections are frequently managed with oral antibiotics, while deep infections typically require surgical debridement (removal of dead, damaged, or infected tissue) and IV antibiotics. A small percentage of infections may be complicated by large soft tissue defects and compromised host immune systems, requiring extensive and prolonged treatments and surgical procedures.
Although major complications are rare, they are more likely to be seen in patients with complicated cases and have been reported to occur in as many as 28% to 32% of adult deformity cases.1 These include complications that are device-related (2% to 5%), neurologic (1% to 2%), vascular (3% to 4%), medical (>10%), stroke (2%), and include death (0.8%).1,2 Sentinel events (relatively infrequent, clear-cut events that occur independently of a patient's condition), including bowel or peritoneal injury, neurovascular injury, wrong site surgery, and retention of a foreign body, occur in 0.8/1,000 cases.3
Both major complications and sentinel events frequently require further medical interventions, resulting in longer hospitalizations, greater costs, and increased mortality.
In the summary years of 2008 to 2011, there were 261,900 hospital discharges or outpatient visits for complications related to spine surgery. These were evenly distributed between men and woman, with an average age in the mid- to late 40s. Health care visits occurred most frequently in the population under age 18 years, and least frequently among persons age 65 years and older.
In addition, there were 1.87 million patient visits related to spinal infections. The majority of the spinal infection diagnoses were for discitis, an infection in the small spaces between the vertebrae of the spine. Only 1% of diagnoses treated in 2010 were to those under the age of 18 years. (Reference Table 3.1.1 PDF [5] CSV [6] and Table 3.1.2 PDF [7] CSV [8])
Postsurgical infections, which are not isolated to spinal surgeries, accounted for 290,400 hospital discharges in 2011, and 217,600 emergency department visits in 2010, of which 63% were admitted to the hospital. Postsurgical infections were most commonly found in persons age 45 to 64 years. (Reference Table 3.2.1 PDF [9] CSV [10])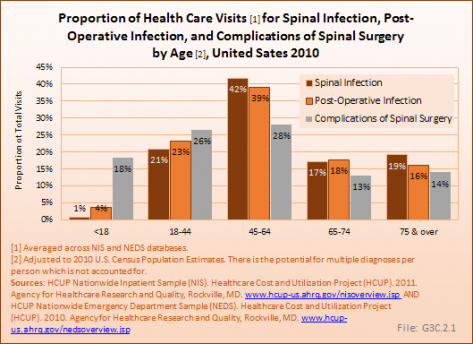
The majority of health care visits for both spinal infection and complications of spinal surgery were to a physician's office, but 22% of cases for complications from spinal surgery resulted in re-hospitalization. (Reference Table 3.1.1 PDF [5] CSV [6] and Table 3.3.2 PDF [11] CSV [12])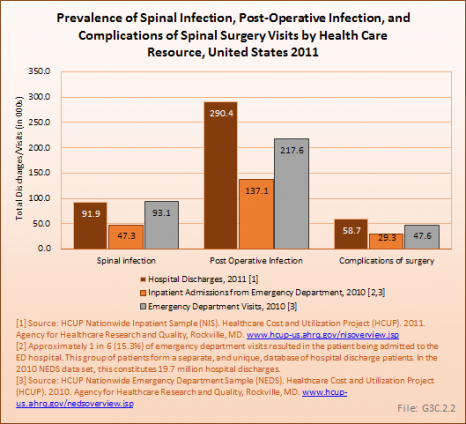
The average length of hospital stay (LOS) for infections and complications were 9.9 days and 8.8 days, respectively. Mean hospital charges for infections and complications were $76,100 and $92,000, respectively. Mean charges for complications of spinal surgery were second highest of all spinal deformity conditions evaluated. Charges related to males were higher than for females for both conditions, and were highest for the youngest patients, those age 17 years and younger. (Reference Table 3.4.1 PDF [13] CSV [14])
In 2011, total costs for patients discharged from a hospital with a diagnosis of either spinal infection or complications of spinal surgery were $12.4 billion. Hospital charges related to postsurgical infections were more than $25.5 billion. These estimates encompass hospital charges only; they do not include other direct costs such as physician charges, outpatient ancillary services, physical therapy, injections, or indirect costs including lost workdays and income. (Reference Table 3.4.4 PDF [15] CSV [16])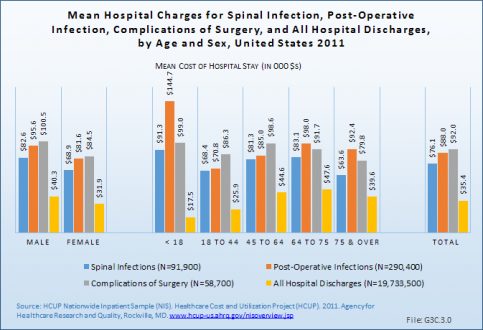
About one-half of patients treated for infection and complications were discharged to home (44% and 62%, respectively), but a substantial proportion were transferred to a long-term facility (29% and 16%, respectively), adding to the cost of treatment for spinal infection and complications from spinal surgery. Discharge status for postsurgical infection hospitalizations were similar. The likelihood of being transferred home declined with age for all groups, with a third to half of patients discharged to long-term care. One in four received additional home health care, increasing the cost of treating these conditions. (Reference Table 3.3.4 PDF [17] CSV [18])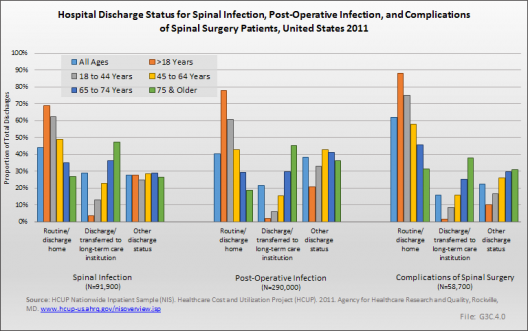
Links:
[1] https://bmus.latticegroup.com/docs/T2.14.pdf
[2] https://bmus.latticegroup.com/docs/T2.14.csv
[3] https://bmus.latticegroup.com/docs/T2.19.pdf
[4] https://bmus.latticegroup.com/docs/T2.19.csv
[5] https://bmus.latticegroup.com/docs/T3.1.1.pdf
[6] https://bmus.latticegroup.com/docs/T3.1.1.csv
[7] https://bmus.latticegroup.com/docs/T3.1.2.pdf
[8] https://bmus.latticegroup.com/docs/T3.1.2.csv
[9] https://bmus.latticegroup.com/docs/T3.2.1.pdf
[10] https://bmus.latticegroup.com/docs/T3.2.1.csv
[11] https://bmus.latticegroup.com/docs/T3.3.2.pdf
[12] https://bmus.latticegroup.com/docs/T3.3.2.csv
[13] https://bmus.latticegroup.com/docs/T3.4.1.pdf
[14] https://bmus.latticegroup.com/docs/T3.4.1.csv
[15] https://bmus.latticegroup.com/docs/T3.4.4.pdf
[16] https://bmus.latticegroup.com/docs/T3.4.4.csv
[17] https://bmus.latticegroup.com/docs/T3.3.4.pdf
[18] https://bmus.latticegroup.com/docs/T3.3.4.csv