

The normal spine viewed from the side forms a gentle "S" shape. When viewed from the back, the normal spine appears straight. The naturally occurring soft curves of the spine are designed to distribute mechanical stress in the body when at rest and during movement. When the curvature is even slightly abnormal, a person may experience occasional mild or annoying discomfort. If the curve is severely abnormal, the pain is usually severe and accompanied by disability. Abnormal curves are referred to as spinal deformities, and include scoliosis, kyphosis, excess lordosis, and flatback.
Spinal deformity and scoliosis can be found at birth due to genetic causes, develop during childhood, or develop late in life because of degenerative disc and joint disease. Common signs of scoliosis are a prominent shoulder or shoulder blade, or chest wall asymmetry. Another sign is uneven hips, with one hip seemingly higher than the other hip. It is important not to confuse scoliosis with poor posture and to realize that scoliosis will usually not disappear with age. In spite of the severity of these conditions and the impact they have on the lives of children, the prevalence of spinal deformities in children under the age of 18 years is difficult to determine because of relatively low numbers and the degree to which the condition manifests initially in pain or disability. Estimated prevalence of spinal deformity conditions has been cited in numerous studies, and ranges from 1 in 1,000 for congenital scoliosis to 68 in 100 for adult spinal deformity or scoliosis for persons age 60 years and older. (Reference Table 3.1.3 PDF [1] CSV [2])
There are several different types of scoliosis. The most common type of scoliosis is idiopathic, meaning the cause of is unknown. Approximately 80% to 85% of scoliosis cases are idiopathic.1 Idiopathic scoliosis can initially occur as early as the first three years of life, which is known as infantile idiopathic scoliosis. If diagnosed between the ages of 4 to 10 years, it is known as juvenile idiopathic scoliosis, and from 10 years of age to skeletal maturity, as adolescent idiopathic scoliosis. Adolescent idiopathic scoliosis is the most common type.
Scoliosis, if severe enough (>25°), is usually treated with bracing if the child is growing, or with surgery if the curvature is more severe (>45° to 50°). The standard radiograph measurement method for all forms of scoliosis is the Cobb angle measurement technique, measured from the end plates of the maximally tilted end vertebral bodies in a standing radiograph.2 Whether the curve is >25° or >40° to 45°, the treatment is preventative in nature, helping to avoid progression of the curve and more significant future problems that might occur if it was left untreated. While this preventative aspect is hugely valuable and intuitively important, its benefit is difficult to measure from a public health standpoint, especially for rare conditions of childhood such as juvenile and adolescent pediatric scoliosis.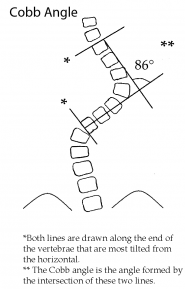
According to the Scoliosis Research Society (SRS), idiopathic scoliosis is diagnosed when a patient has asymmetry on forward bending combined with a curve of at least 10°.1 By this definition, the prevalence of adolescent idiopathic scoliosis in children from 10 to 16 years of age is 2% to3%. Though the male-to-female ratio for smaller curves is about equal, larger curves seem to be more common in females. Similar results were found in a study conducted in 1985, where 29,195 children were screened for idiopathic scoliosis.2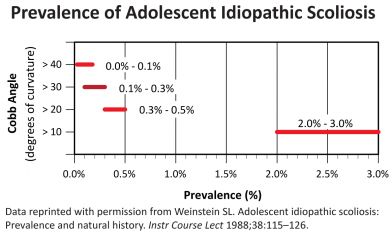
Several studies have investigated the natural history and natural course of curve progression in adolescent idiopathic scoliosis. All report the strongest predictive factors in the development of idiopathic scoliosis are age, magnitude of curve, and gender.3,4,5,6,7 Girls are more likely to have adolescent idiopathic scoliosis than boys, and some studies report the onset is earlier in girls than boys. A factor highly correlated with curve progression is age at diagnosis; patients diagnosed at a younger age have a greater risk of curve progression. However, those diagnosed at a younger age seem to have a more favorable response to milder forms of treatment, which supports the practice of school screening to detect and lead to earlier diagnosis for those children with a smaller degree of curvature.
Treatment decisions for individuals with adolescent idiopathic scoliosis are made based on location, shape, pattern, and cause of the curve. The treatment choice is also a function of the patient’s future growth potential. Treatment choices include observation, bracing, and surgery. Observation is usually reserved for patients who have curves ≤25°. Bracing, which is used to stop curve progression (rather than for lasting correction of the curve), is usually used for patients who have curves ≥25° and who are still growing. Surgery is generally used for patients with curves ≥45°.
In 12% to 21% of idiopathic scoliosis cases, the diagnosis is made between 4 and 10 years of age. Between the ages of 4 and 6 years, the female-to-male ratio of juvenile idiopathic scoliosis is 1:1. However, the ratio of female to male cases rises to between 2:1 and 4:1 in children between the ages of 4 and 10 years, and to 8:1 in children who are 10 years of age or older.1 Both right and left curves are found with equal frequency for patients younger than 6 years, but rise to a 3:1 ratio of right versus left thoracic curves after the age of 6.2
Observation is the main treatment for patients with a small curve of less than 20° to 25°. Follow-up visits are recommended every 4, 6, 9, or 12 months, depending on the patient’s age, the degree of the curve, and the characteristics of the clinical deformity.1
Curves between 25° and 50° are usually treated with bracing in this age group. Bracing can be done either on a part-time or full-time basis, depending on the size of the curve as well as the age of the child. A study completed in 1982 evaluating the success of bracing reported an excellent prognosis when part-time bracing was utilized for patients with a curve of ≤35° and rib-vertebra angle difference (RVAD)3 of ≤20°; however, curves ≥45° and RVAD of ≥20° had a less favorable prognosis for successful treatment with bracing.1
Overall, the curve patterns in patients with juvenile idiopathic scoliosis are similar to those with adolescent idiopathic scoliosis. Approximately 70% of patients with juvenile idiopathic scoliosis exhibit curve progression and require some form of treatment. In a study conducted in 1981, 55 of 98 patients (56%) with juvenile idiopathic scoliosis required spinal surgery. The most common and traditional surgery is posterior instrumentation and fusion.1
Infantile scoliosis currently accounts for less than 1% of all cases of idiopathic scoliosis in the United States. Boys are affected by infantile idiopathic scoliosis at a higher rate than girls (3:2 ratio).1 Infantile scoliosis curves tend to be left-sided (75% to 90%). Past studies have indicated this rare type of scoliosis occurs more frequently in Europe than in North America.2
Treatment for patients with infantile idiopathic scoliosis is determined by anticipated or actual curve progression. Several common measurement techniques are used, with angles ≤20° generally considered at low risk for progression. Re-evaluation is recommended every 4 to 6 months.1
In addition to measuring the Cobb angle, the RVAD is used as a common predictor of curve progression.3 Patients with a Cobb angle of ≤25° and a RVAD of ≤20° are at a low risk for progression and should be re-evaluated every 4 to 6 months.1
Nonsurgical treatment, such as bracing or casting is initiated if a curve progression of ≥10° occurs. Surgical treatment should be considered when nonsurgical measures, including both bracing and casting, are not successful. Surgical treatment is utilized when a curve is ≥45° and progressive in an immature child.1 Overall, surgical methods are continually evolving, with the goal of obtaining and maintaining curve correction while simultaneously preserving or encouraging spinal and trunk growth.
Surgical options currently utilized include various types of spinal fusion or hemiepiphysiodesis, a minimally invasive implant procedure to slow progression of curve growth. Additional techniques include growing-rod instrumentation (rods that expand and support the deformed spine) and vertical expandable (telescoping) prosthetic titanium rib (VEPTR) instrumentation.4The goal of using surgical methods is to halt the progression of the curve and gain correction of the deformity, allowing maximum growth of the spine, lungs, and thoracic cage.1
Congenital scoliosis is believed to affect approximately one child for every 1,000 live births.1 The cause is unknown in most cases, but in some cases, it is associated with various syndromes, as shown in the illustration below. Diagnosis occasionally is made during prenatal ultrasound. In cases of congenital scoliosis, additional congenital conditions, such as chest wall malformation or kidney or heart abnormalities, are often present. Treatment options for congenital scoliosis are bracing and/or surgery, and are similar to those discussed for idiopathic scoliosis. Bracing is not as effective for congenital scoliosis as it is for idiopathic scoliosis.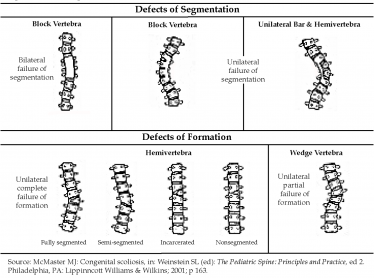
Major abnormal spinal deformity presenting during infancy or early childhood poses a clinical problem because of the anticipated long growth period (at least 10 years), variable presentation and treatment methods, and the length of time that must pass before meaningful outcome results can be assessed in the small number of patients for definitive studies. Curves that result from congenital scoliosis are often not treated as easily as idiopathic curves because the deformity is in the bones rather than the soft tissue, causing the curve to be rigid.2
Scoliosis also occurs in conjunction with several congenital conditions that occur in infancy or childhood. These include muscular dystrophy, cerebral palsy, spina bifida, and spinal muscular atrophy. Scoliosis associated with these conditions is referred to as neuromuscular scoliosis. Both the likelihood and the severity of the scoliosis generally increases with the severity of the underlying condition. For example, a child with severe cerebral palsy who is unable to walk is more likely to have severe scoliosis than a child with mild cerebral palsy who can walk.
Because of the low prevalence of scoliosis in children and adolescents, analysis of the health care impact this condition causes is difficult. However, the impact of scoliosis over a lifetime in terms of pain, inability to work, and cost to the health care system are substantial.
In 2010–2011, 92% of the 663,700 health care visits with a diagnosis of scoliosis for those under the age of 18 years were classified as idiopathic scoliosis. The majority (94%) were outpatient visits to either an outpatient clinic or physician office. Only 3% represented hospital discharges; however, this still accounted for 20,100 discharges for this often painful condition in children and adolescents. (Reference Table 3.1.2 PDF [6] CSV [7])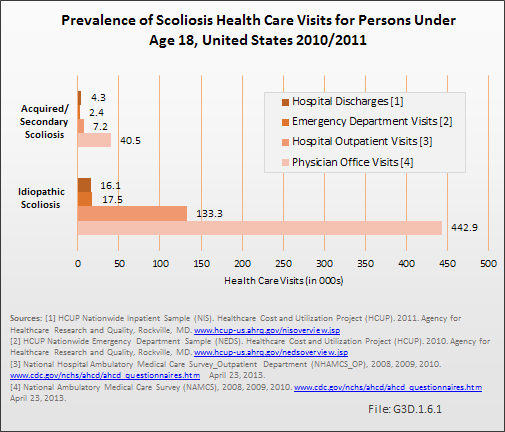
In 2011, 42% of children and adolescents under the age of 18 years discharged from the hospital with a diagnosis of scoliosis had surgery. Spinal fusion was the most common surgery performed, followed by instrumentation and decompression. Of those having surgery, three-fourths (78%) had only one type of surgery. However, one in five had two or all three types of surgery. Reference Table 3.5.1 PDF [8] CSV [9])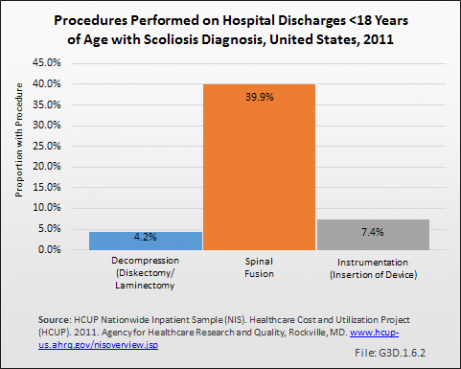
Average hospital charges for patients with scoliosis under 18 years of age who had surgery in 2011 were four or more times the average for all scoliosis patients in this age group, even though the length of stay was only about 50% longer. Patients who had an instrumentation procedure had the highest average charges of $165,600, although this may have been in conjunction with another procedure.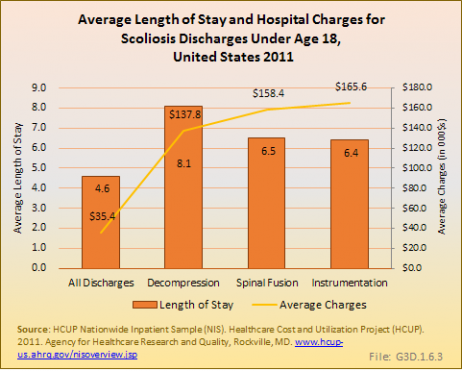
Deformity of the adult spine includes patients with curvature of the spine (scoliosis) of varying degrees caused or impacted by degenerative disc and joint disease. Adult scoliosis may be the result of persistent or progressive deformity since adolescence or a new, de novo, onset of deformity resulting from degeneration or aging of the spine. Degenerative scoliosis accounts for the majority of scoliosis cases in older populations aged 65 years and older, as reflected in the low proportion of older patients with a diagnosis of primary idiopathic scoliosis.
Degenerative scoliosis is one of the most challenging spine conditions to treat because of the variability of the condition. Generally, it is thought to originate with the degeneration of the intervertebral discs, which leads to misalignment of the vertebral column. Degenerative scoliosis, particularly in the very elderly, is often associated with other conditions, such as osteoporosis. Treatment outcomes for both nonsurgical and surgical procedures are not well documented; hence, recognition and earlier intervention are important to ward off the more complex problems of adult scoliosis. The role played by undiagnosed, mild idiopathic adolescent scoliosis on the development of degenerative scoliosis in later life is unknown.
While scoliosis is the primary form of spinal curvature, two other spine curvature disorders are included in the data cited here. These are lordosis, also known as swayback, where the spine curves significantly inward at the lower back, and kyphosis, characterized by an abnormally rounded upper back with a curvature of more than 50º.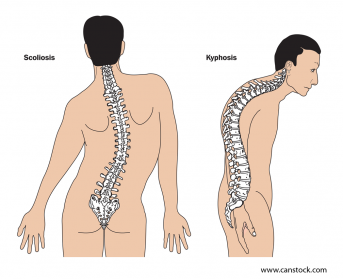
The clinical presentation and management of adults with scoliosis is characterized by a great deal of variability. There is a poor correlation between the magnitude of deformity and the impact of scoliosis on health status, as patients with large spinal curvatures may have limited pain and disability with and patients with relatively mild deformity may be severely impaired. Deformity in the sagittal plane (lateral) is most closely associated with disability.1 Patients with adult scoliosis seek medical care for symptoms including back pain, neural symptoms, and progression of deformity.
The prevalence of adult spinal deformity and scoliosis is not well established, with estimates ranging from 2.5% to 25% of the population.1,2,3,4,5,6 A 2005 study reported mild to severe adult scoliosis prevalence as high as 68% in a healthy (no known scoliosis or spine surgery) population aged 60 years and older.7 Many cases of degenerative scoliosis are undiagnosed, but elderly patients often seek care because of back and leg pain that may be caused by scoliosis and associated spinal stenosis.
According to 2010 US Census Population Estimate, there were 235,205,658 people in the United States over the age of 18 years. Prevalence of adult scoliosis cited in the literature ranges from 2.5% to 60%, depending on severity. A conservative estimate (2.5%) of the prevalence of adult scoliosis yields an incidence of a minimum of 5.88 million adults in the United States with adult scoliosis. In 2010–2011, an estimated 1.61 million of these adults received treatment either as an inpatient or on an outpatient basis. (Reference Table 3.1.2 PDF [6] CSV [7])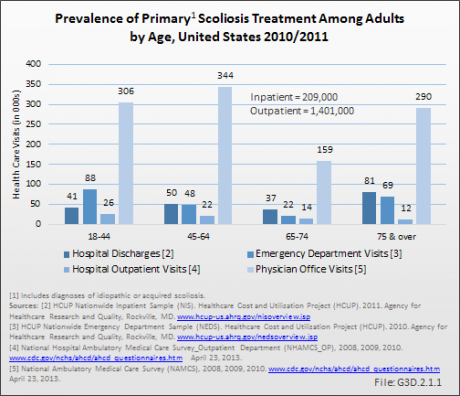
Estimates for prevalence of lordosis or kyphosis as the primary diagnoses is approximately 17% of spine curvature diagnoses in hospital and emergency departments, with patient hospital discharges higher (23%). (Reference Table 3.2.2 PDF [10] CSV [11])
The management of adult scoliosis includes nonsurgical and surgical resources. Nonsurgical treatments of adult scoliosis utilize significant resources, and include interventions such as exercises, physical therapy, injections, pain medications, and manual manipulation.1 Data on nonsurgical treatments is not available; however, a 2010 non-randomized study reported that two years of nonsurgical treatment in adult scoliosis patients resulted in substantial expenditures and yielded no improvement in health status.2
Operative management of scoliosis in the adult encompasses a spectrum of procedures including decompression alone, decompression with limited fusion, and fusion of the deformity. In 2011, a query of the Healthcare Costs and Utilization Project (HCUP) Nationwide Inpatient Survey (NIS) resulted in approximately 229,100 hospitalizations associated with a discharge diagnosis of scoliosis or spinal curvature (ICD-9-CM of 373). The majority of these, or 155,900 patients, were diagnosed as idiopathic scoliosis, or scoliosis of unknown cause. Most of the remaining discharges, 66,000 people, were associated with a primary diagnosis of acquired adult scoliosis, while the remaining 10,500 discharges were associated with adult scoliosis as the secondary diagnosis to another condition. (Reference Table 3.1.1 PDF [12] CSV [13])
In 2011, nearly 27.6 thousand patients admitted to the hospital with a diagnosis of scoliosis underwent a decompression procedure. Among patients having decompression, 82% also had spinal fusion, with 42% undergoing fusion of one to three levels, while 34% had fusion of four or more levels. Overall, 22% of all scoliosis patients underwent a fusion procedure (N=50,009), with 10% having fusion of one to three levels and 12% fusion of four or more levels.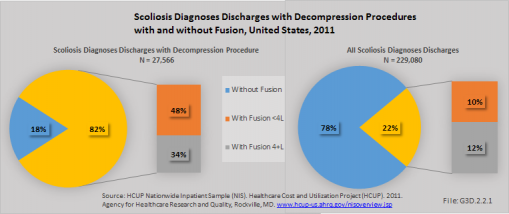
In 2011, only about one-half (53%) of patients with a scoliosis diagnosis were discharged to home, while 70% of patients discharged for any diagnosis had a routine discharge. Patients with a scoliosis diagnosis are more likely to be transferred to a skilled nursing or intermediate care facility than are patients with all diagnoses. This is particularly true for the elderly population, with 46% of persons age 75 and older with a scoliosis diagnosis moving to a long-term care facility. (Reference Table 3.3.1 PDF [14] CSV [15])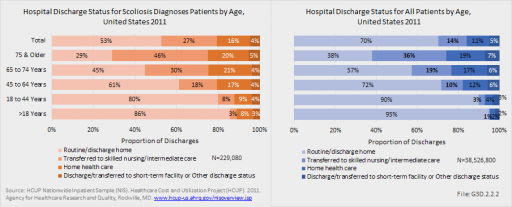
The cost of care for adults with scoliosis includes direct costs and indirect costs including lost wages, time from work, cost of care providers, and opportunity costs. Estimates of the direct costs of nonsurgical care in adult scoliosis are estimated to be as high as $14,000 per year.1
The national mean cost of a hospitalization (presumably for surgical treatment) for patients with a primary diagnosis of idiopathic scoliosis was $67,400 in 2011 for an average hospital stay of 5.6 days. The HCUP NIS database does not provide hospitalization costs associated with secondary discharge diagnoses, and does not include fees to doctors, tests, and other typical charges associated with hospitalization. Therefore, the most conservative estimate of only the hospitalization cost for adult scoliosis in 2011 was an estimated $15.44 million (229,000 hospitalizations). The real cost of the management of adult scoliosis to our healthcare system is significant, and the value of care measured by change in health status remains incompletely defined for both nonsurgical and surgical care. (Reference Table 3.4.1 PDF [16] CSV [17])
Mean charges for scoliosis diagnosed patients are similar to those for other spinal deformity diagnoses, but significantly higher than for all hospital discharge patients.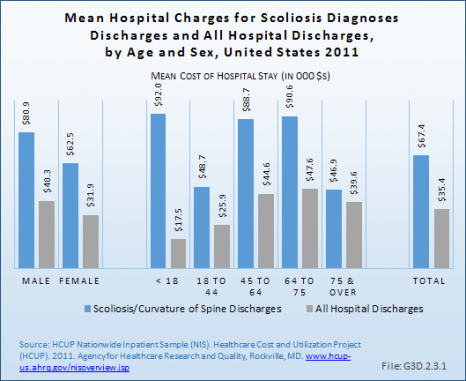
While technical outcomes of surgery are well known and show obvious benefits for those with significant deformity, long-term health related outcomes have yet to be precisely documented. The lack of quality, long-term studies of sufficient size hampers our understanding of the mortality and morbidity rates for patients with congenital and idiopathic scoliosis, with and without treatment. Fifty years of follow-up studies of children and adolescents with untreated scoliosis have shown conflicting results, with some studies indicating a higher risk of mortality and respiratory compromise.1,2
Another study shows compromise only in patients with early reduced lung function and a large curvature.3 Yet another study has shown no differences in untreated childhood scoliosis and a control group.4 Several articles from the 1960s and one recent article report that low back pain does not occur more frequently in untreated scoliosis patients than in the general population4,5,6 unless the curvature is greater than 40°.7,8 It has also been shown that persons treated with surgery rather than bracing for adolescent idiopathic scoliosis have less pain at 10- to 20-year follow-up, although function remains similar.9,10 The cosmetic/self-image aspect of scoliosis is obvious and important, and often a major factor affecting the lives of individuals with this condition.
Links:
[1] https://bmus.latticegroup.com/docs/T3.1.3.pdf
[2] https://bmus.latticegroup.com/docs/T3.1.3.csv
[3] http://www.niams.nih.gov/Health_Info/Scoliosis/default.asp
[4] http://www.wheelessonline.com/ortho/congenital_scoliosis_and_vertebral_defects
[5] http://www.ncbi.nlm.nih.gov/pubmed/15931035
[6] https://bmus.latticegroup.com/docs/T3.1.2.pdf
[7] https://bmus.latticegroup.com/docs/T3.1.2.csv
[8] https://bmus.latticegroup.com/docs/T3.5.1.pdf
[9] https://bmus.latticegroup.com/docs/T3.5.1.csv
[10] https://bmus.latticegroup.com/docs/T3.2.2.pdf
[11] https://bmus.latticegroup.com/docs/T3.2.2.csv
[12] https://bmus.latticegroup.com/docs/T3.1.1.pdf
[13] https://bmus.latticegroup.com/docs/T3.1.1.csv
[14] https://bmus.latticegroup.com/docs/T3.3.1.pdf
[15] https://bmus.latticegroup.com/docs/T3.3.1.csv
[16] https://bmus.latticegroup.com/docs/T3.4.1.pdf
[17] https://bmus.latticegroup.com/docs/T3.4.1.csv