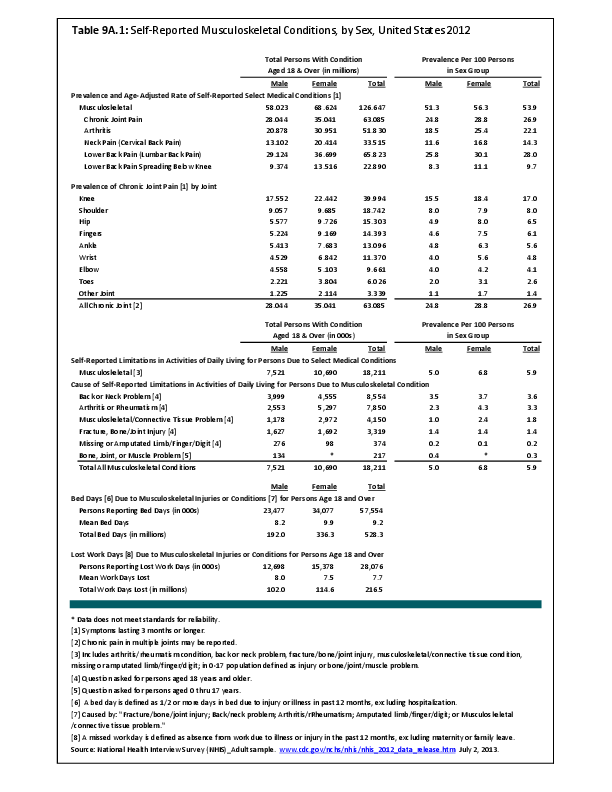
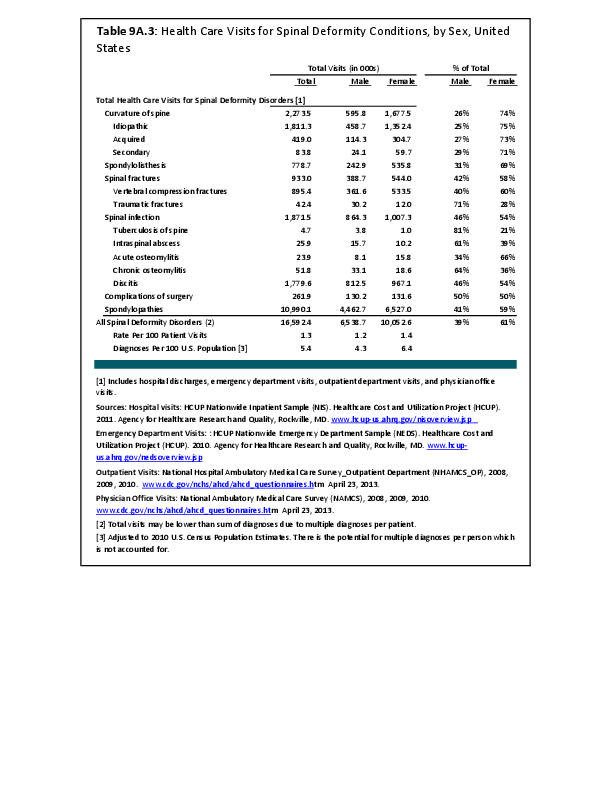
Sex-based differences in incidence and presentation have been described for some, but not all, conditions of the spine. For example, adolescent idiopathic scoliosis, one of the most common diseases of the spine in adolescence, is somewhat more common in females, and females are much more likely to present with larger curves. The incidence of scoliosis among adults, which includes a wider range of diagnoses than adolescent idiopathic scoliosis, does not appear to differ by sex, and there appears to be no sex-based differences in magnitude of curves.1 Ankylosing spondylitis is diagnosed more frequently in men. However, women who present with this condition tend to be older than their male counterparts, have a shorter duration of disease, be more likely to have thoracic spine involvement, and be less likely to be HLA-B27 positive.2
Among the common conditions of the spine, data are often conflicting regarding any sex-based differences in incidence, most likely reflecting their multifactorial etiology. Degenerative disc disease and lumbar radiculopathy, for example, have been reported to be more common in men, more common in women, or equal in lifetime sex-based risk. Women with degenerative disc disease have been noted to present with this condition when they are approximately 10 years older than men,3 perhaps reflecting differences in activity and mechanical loading. Among a young active military population, degenerative disc disease4 and lumbar radiculopathy5 were found to be more common among women, although female sex was less of a risk factor than older age for both conditions.
A variety of risk factors have been described to account for any noted sex-based differences among spine conditions. The most obvious difference would be the influence of sex hormones. Studies related to hormones and spinal deformity, which is more common in women, have shown no clear relationship, while in cases of ankylosing spondylitis, which is more common in men, studies have shown no differences in adrenal or gonadal sex hormones6 to explain this predominance.
As with other conditions, any sex-based differences are likely multifactorial. Schoenfeld5 postulated that these differences might reflect hormonal influences as well as differing responses of the spine to loading and physical activity. Among a cohort of asymptomatic young adults,7 it was found that the spine from T1-L5/S1 as a whole, and the individual high thoracic and lumbar vertebrae, were more dorsally inclined in women than in men. The authors hypothesized that this could make the spine less rotationally stable in women, in certain circumstances resulting in the initiation and/or progression of spinal conditions, such as scoliosis.
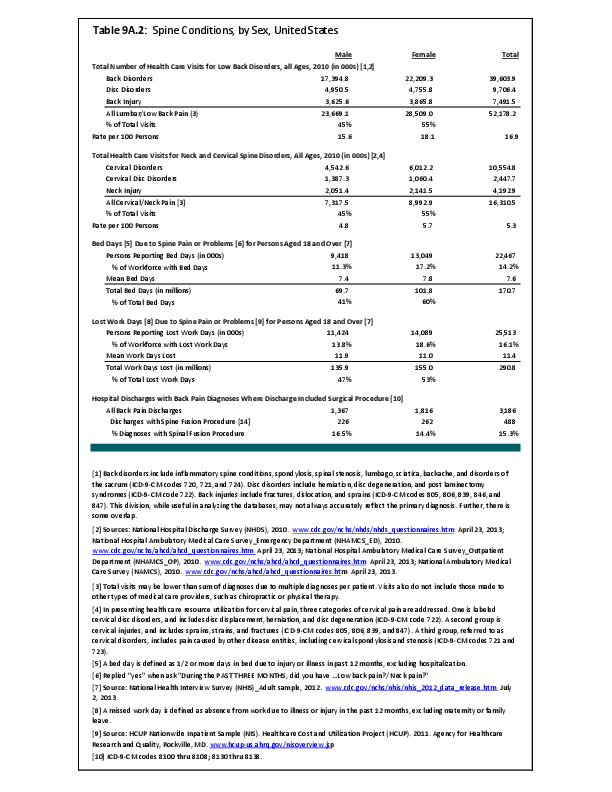
The potential impact of sex on other spine conditions has also been studied, without conclusive results. Increased paraspinous muscle degeneration has been suggested to correlate with incidence of low back pain,8,9 and in studying a cohort of symptomatic adult patients, it was found that women were more likely than men to demonstrate fatty infiltration of their paraspinous muscles on MRI. Sex-based differences have also been identified in paraspinous muscle fiber and type.10 However, the impact of sex on the development of low back pain. and any cause-and-effect relationship between low back pain or other spine conditions and changes in paraspinous muscle composition, has not been elucidated.
- 1. Kebaish KM, Neubauer PR, Voros GD, et al: Scoliosis in adults aged forty years and older: Prevalence and relationship to age, race, and gender. Spine 2011 Apr 20;36(9):731-736. doi: 10.1097/BRS.0b013e3181e9f120.
- 2. van der Horst-Bruinsma IE1, Zack DJ, Szumski A, Koenig AS: Female patients with ankylosing spondylitis: Analysis of the impact of gender across treatment studies. Ann Rheum Dis 2013 Jul;72(7):1221-1224. Epub 2012 Dec 22.
- 3. Battie MC, Videman T: Lumbar disc degeneration: Epidemiology and genetics. JBJS-A 2006;88(Supple 2):3-9.
- 4. Schoenfeld AJ, Nelson JH, Burks R, Belmont PJ Jr: Incidence and risk factors for lumbar degenerative disc disease in the United States military 1999-2008. Mil Med 2011 Nov;176(11):1320-1324.
- 5. a. b. Schoenfeld AJ, George AA, Bader JO, Caram PM Jr: Incidence and epidemiology of cervical radiculopathy in the United States military: 2000 to 2009. J Spinal Disord Tech 2012 Feb;25(1):17-22. doi: 10.1097/BSD.0b013e31820d77ea.
- 6. Straub RH, Struhárová S, Schölmerich J, Härle P: No alterations of serum levels of adrenal and gonadal hormones in patients with ankylosing spondylitis. Clin Exp Rheumatol 2002 Nov-Dec;20(6 Suppl 28):S52-S59.
- 7. Janssen MM, Drevelle X, Humbert L, et al: Differences in male and female spino-pelvic alignment in asymptomatic young adults: A three-dimensional analysis using upright low-dose digital biplanar X-rays. Spine 2009 Nov 1;34(23):E826-E832.
- 8. Mengiardi B, Schmid MR, Boos N, et al: Fat content of lumbar paraspinal muscles in patients with chronic low back pain and in asymptomatic volunteers: Quantification with MR spectroscopy. Radiology 2006 Sep;240(3):786-792.
- 9. Nam WD, Chang BS, Lee, CK, Cho JH: Clinical and radiological predictive factors to be related with the degree of lumbar back muscle degeneration: Difference by gender. Clinics in Orthopedic Surgery 2014;6:318-332. doi: 10.4055/cios.2014.6.3.318. Epub 2014 Aug 5.
- 10. Doherty TJ: The influence of aging and sex on skeletal muscle mass and strength. Curr Opin Clin Nutr Metab Care 2001;4(6):503-508.
Edition:
- 2014

 Download as CSV
Download as CSV